Three key insights I gained from working on SH:24
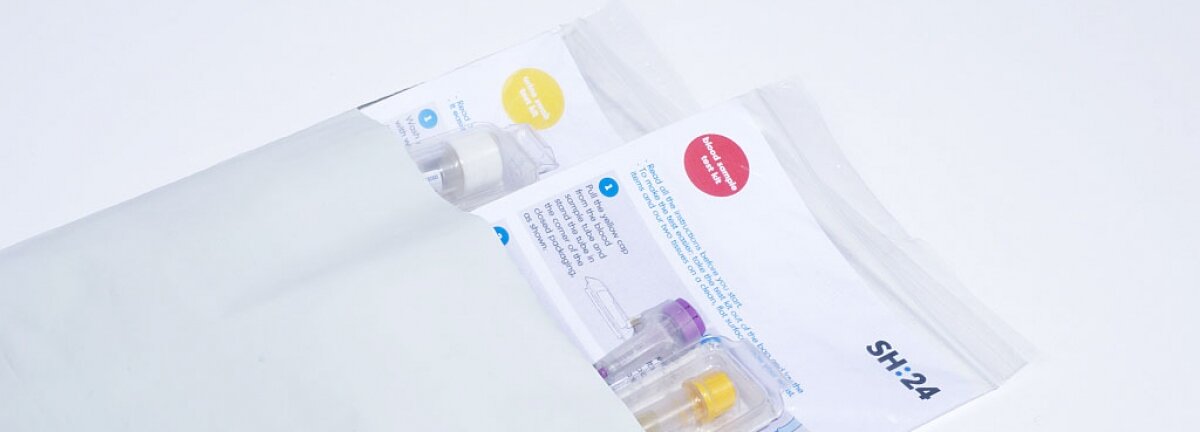
SH:24 is an online sexual health service that launched in March, delivered in partnership with the NHS. The service provides people in Southwark and Lambeth with free STI test kits, information and advice - 24 hours a day. Design Council are a long term partner and have a seat on SH:24’s advisory board.
Designer Mollie Courtenay has worked with Chris Howroyd, SH:24 Design Lead, throughout the discovery stage and is currently helping to optimise the service. Here she shares her thoughts on the project.
I first become involved with SH:24 in February 2013. Chris and I mapped out a user journey for ordering a STI test kit online. We then compiled a list of 12 key assumptions that we needed to test during a discovery phase.
A year later, we have publicly launched a service that we’re confident caters to our users’ needs and wants.
These are three key insights I gained from working on the project:
1. Patients’ opinions are essential to the design process
I spent many days speaking with individual patients in the waiting rooms of Camberwell and Burrell Street clinics, trying to gauge how much they’d want SH:24 to be visually linked to the NHS, among other things.
Most people said that if SH:24 was not associated with the NHS, they would not use it. Some also said that a link to the NHS would mean that they could trust the service to keep their personal information confidential. Quality, credibility and free services/tests were all related to the NHS brand.
While users were keen to see a visual link between SH:24 and the NHS, a distinct SH:24 brand was desirable too. Many suggested avoiding the traditional ‘NHS blue’, suggesting it could come across as too clinical.
2. Clinical staff perspectives are equally important
I took clinical staff - including receptionists, health advisors and band six nurses - through the same user journey map as the one I used with patients.
Some of the more memorable insights from these discussions with clinicians included the following:
- Downloadable/printable results would be useful for sex workers - a high risk group.
- Visual instructions are key
One Health Advisor believed that people rarely read the instructions for the DIY tests - often they guess and sometimes ‘it can go very wrong’. - The need to make it clear that neither SH:24 or the clinics would not share patients’ data - either with GPs or other care providers - and that their details would not be linked to NHS numbers.
Clinicians are aware lots of people do not know this when they visit the clinic and some think it is a barrier to attending. Certain younger people I spoke with did have concerns that their sexual health record would be linked to the health record at their family doctor.
3. Strong team communication is vital
As we worked in short sprints with a constantly growing SH:24 team, we found it helpful to use a number of tools and services to keep up with activity.
To manage day-to-day communication between team members near and far, we agreed to use Slack. We used channels to split conversations by topic and get quick feedback from the team on visuals.
Trello helped us to manage the backlog and tasks for each sprint. We set up boards for individual elements of the front or back-end, left questions for each other and recorded insights from user interactions. This combined to create a really useful narrative of our learning and progress that is great to look back on now.
We also used Google Drive for document sharing and Google Hangouts for morning stand-ups when we weren’t physically in the same room.
Looking ahead
What I have learnt most of all from SH:24 is that internal and external communications need to be made accessible, empathetic and enabling for all.
We hope that SH:24 will act as an exemplary project, showcasing how complex, multi-stakeholder services can be delivered innovatively, while improving users’ health outcomes.
Subscribe to our newsletter
Want to keep up with the latest from the Design Council?
